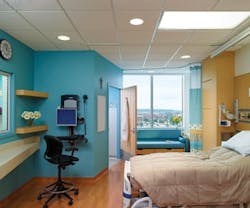
While no one likes to go to the hospital, the good news is that modern patients are being treated in some of the most comfortable, accommodating settings ever created.
Thanks to the patient-centered model of care and evidence-based design, patient rooms have evolved from small, multiple-occupancy spaces into spacious, single-occupancy suites, reducing the spread of infection and increasing patient satisfaction. Large windows and warm textures provide a touch of home, while high-tech additions such as flat-panel televisions and mobile docking stations add to the happiness quotient.
And so, as healthcare designers work to bring the things that patients find comforting closer to the bedside, it was perhaps inevitable that the nursing staff would soon follow. Over the course of the past decade, enterprising designers have downsized the traditional, centralized nurse station—formerly the heart of a hospital unit—and replaced it with smaller alcoves and workstations situated closer to the patients.
Now commonly known as decentralized nursing or caregiving, this shift has resulted in more direct care and taken a bite out of the 4.1 miles the average ward nurse walks in a day (assuming a three-patient assignment, as stated in a 2006 study by Welker, Decker, Adam and Zone-Smith). Its well-noted effects on patient and staff well-being have already made it a near-standard, not only among healthcare designers but hospital officials as well.
“In the hospital setting, it’s more than just the physical translation of a central nurse station versus satellite stations,” says John Rodenbeck, AIA, associate principal and healthcare architect with Perkins Eastman. “It’s really evolved into [the hospital’s] definition of a model of care. I think that most nursing administrators, when they talk about decentralized nursing, they’re really talking about the way that their nurses are delivering care. There’s a closer proximity of caregiving to the patient.”
Of course, as with any emerging model of care, there remain plenty of unanswered questions. What role does the environment have on nurse burnout, and can decentralization help? Will noise increase in patient areas without a central hub for staff members? Will nurses be distracted? To understand the range of issues surrounding this trend, we asked designers from three well-respected firms about their experiences with decentralized nursing, and in the process, discovered just how much the model continues to evolve.
FROM THEN TO NOW
The decentralization model has made its biggest mark in the past decade, but what is interesting is just how far back the concept’s underlying ideas go—and how they can be traced to one man in particular.
Gordon A. Friesen, perhaps one of the first true healthcare consultants, spent the better part of his life working to improve healthcare supply chains. He believed that a nurse’s primary duty was to be available to the patient at all times; in order to accommodate this, Friesen advocated placing every supply and medication needed by a nurse at the patient’s bedside. This gave rise to a variety of innovations in patient room design in the 1960s, including the nurseserver, a supply closet inside the patient room that could be stocked from the corridor.
Unfortunately, a host of issues ranging from pushback by fire marshals to inventory problems caused Friesen’s ideas to fall out of favor by the 1970s, although Gary Nyberg, AIA, healthcare principal with HGA, says one of the biggest reasons boiled down to sheer efficiency.
“The reason it went away was the tyranny of paper, so to speak,” he says. “There needed to be a central spot for the medical records to be kept, and the centralized nurse station was a reaction to that.”
Fortunately, mobile technologies and working electronic medical records have brought decentralized nursing back into vogue, and it turns out that it couldn’t have happened at a better time. Patients are coming into hospitals sicker and with more complex cases, requiring more attention from nursing staffs. Likewise, as sizable single-patient rooms have become the new norm, the average hospital floorplate has increased, increasing the physical toll on caregivers.
Decentralization tackles both of these problems by positioning satellite stations just outside of patient rooms—typically between two rooms to aid in supervision—or inside the patient rooms themselves. While these stations vary from facility to facility, they may feature a writing surface, computer access, basic storage and even hand-washing stations. Many models also bring the storage of commonly used supplies directly inside a patient’s room—with some even reviving Friesen’s nurseserver concept—or locate storage rooms within a short distance of the patient.
“When you’re planning the unit, you have to think about the storage of equipment that will make [nurses’] lives easier,” says Susan DiMotta, IIDA, AAHID, principal and senior living interior designer with Perkins Eastman. “The fewer steps that they have to do, the less they have to think about and remember where things are, the easier you make their lives.”
That’s not to say that the model is a panacea. While it may ease the physical burden on caregivers—a primary reason that nurses leave the healthcare field, according to a 2001 survey by Peter D. Hart Research Associates—some nurses have complained that decentralization leaves them feeling disconnected and isolated from their co-workers. Concerns about staff turnover have brought these concerns to the forefront of healthcare design.
“[Nurses] need to collaborate with each other—they’re accustomed to that, and it’s an aspect of nursing that many nurses enjoy,” says Jocelyn Stroupe, AAHID, IIDA, ASID, EDAC, principal, healthcare interiors practice leader with Cannon Design. “We’ve started to create spaces that address the emotional and physical needs of nurses, now more than ever before.”
Many designs now rely on a hybrid model that blends satellite stations with a central, but smaller, nurse hub, allowing staff to spread out for patient care, but still meet for collaboration or a break. In both hybrid and fully decentralized models, designers have also begun including a variety of back- or off-stage spaces for the nursing staff, which function in the same way. But while nursing lounges used to be buried in amongst other support spaces, this new breed of lounge is infused with natural light and filled with comfortable furnishings. Designers have also begun incorporating quiet zones or workstations into decentralized units for focused, concentrated work, and entire quiet rooms for decompression and reflection.
These backstage spaces also help reduce the noise generated in decentralized corridors, allowing nurses, physicians and families to talk in a private setting instead of in hallways of outside patient rooms. Advances in antimicrobial technology have also made it possible to carpet corridors, further reducing sound levels, while some firms have begun designing entirely separate traffic paths for caregivers and patients, and support staff and equipment.
As for concerns that satellite stations lack the necessary space for nurses to do administrative work, the designers interviewed said that electronic medical records have largely made that a moot point. However, there is a new emphasis on providing supportive work spaces for whatever type of work a nurse might be doing. Ergonomic seating, adjustable task surfaces and lighting are all making the jump from the office to the hospital ward.
“No two nurses are alike, just like no two patients are alike,” says Madhu Gresla, vice president with Cannon Design. “We want to create environments that are flexible enough to accommodate all of the needs of all types of caregivers. To label it centralized or decentralized is, I think, beside the point—we’re trying to make workstations and teaming environments that allow for the flexibility of caregiving.”
the future of decentralization
So what does the future hold for the decentralized model of care? All evidence points to its continued spread through the healthcare industry as its benefits to patients and staff continue to be discovered, and technology will continue to play a big part in that. What isn’t as certain is the exact form it will take. According to Nyberg, “there’s a goal to push the envelope a little bit further,” in terms of bringing
more to the bedside, including computers and meds, and many forward-thinking hospitals are experimenting with these ideas. However, concerns among administrators about controlling narcotics access and the spread of infection have also caused some hospitals to pause and reconsider.
“We can’t underestimate the importance of infection control, especially in acute care environments,” says Rodenbeck. “That in itself has sort of begun to dictate where documentation stations are and what is actually permitted to be brought into the room. I’m seeing more reluctance to use COWs [computers on wheels]—for a period of time it was a very convenient and flexible solution. Infection control is now saying no, they don’t want this mobile model going from room to room, because that’s going to spread infection.”
Similarly, while design firms have begun experimenting with charting and nurse stations directly in patient rooms, some healthcare facilities have chosen to tread slowly, worried about interruptions and medical errors.
“I think you’ll find the cultures of different organizations are going to be big drivers of how things go,” Stroupe says. “I’ve had some facilities
really push back against charting in the room, because some nurses don’t feel comfortable with the family watching them while they do it, or maybe they feel like they’re too distracted doing it there. [A culture’s mindset] is a significant component, and as designers, it’s important for us to understand that.”
Stroupe adds that while the future of the decentralized model will likely be shaped by further advancements in technology and our understanding of the healing process, for now, it will rely on designers working closely with nursing staffs to understand their needs, while suggesting improvements that may improve satisfaction or workflow.
“We don’t want to just replicate the same thing that we’ve always done just because they’re comfortable with that, but at the same time, you need to test that tolerance and get them to really buy into doing something new.”